
The catheter ports are flushed with sterile saline and the catheter is introduced over the top of the guidewire, holding the guidewire with one hand, and advancing the catheter over it with the other. This is then removed again, leaving the guidewire in situ. 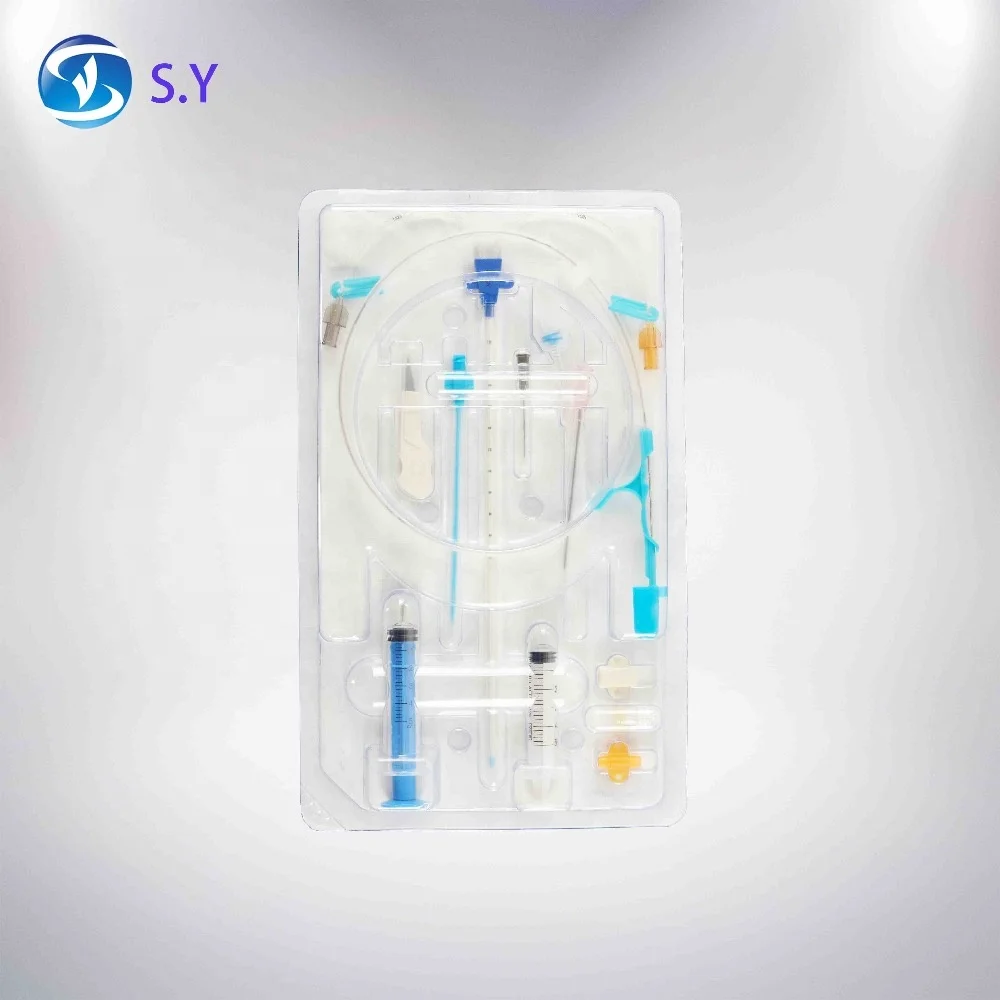
The introducer and peripheral IV catheter are removed, leaving the guidewire in situ.Ī dilator is placed over the top of the guidewire, to facilitate the introduction of the catheter. The anaesthetist should monitor the patient’s ECG closely during this time, as cardiac arrhythmias can be seen if the guidewire is advanced too far into the cranial vena cava. Approximately 20-30cm of guidewire should remain outside of the patient’s vein, depending on the length of the guidewire and catheter being used. If using the Seldinger technique, the guidewire introducer is placed into the catheter hub, and the guidewire advanced using the measuring markers on the wire as a guide. Using the large-bore peripheral IV catheter supplied in the jugular catheter kit, the jugular vein is cannulated, the stylet removed, and the catheter bunged. Two versions are available Seldinger (guidewire) technique or peel-away techniqueĬhloraprep or final skin preparation applicatorĪ 10x10 cm area is clipped over the right jugular vein (typically the left is not used if possible, as oesophagostomy tubes are placed on this side) and aseptically prepared.Ī small stab incision is made in the skin over the jugular vein. Jugular catheter kit of appropriate size and length, based on patient Kinking of the catheter, complicating administration of fluids or medications – careful selection of the placement and suture site is advised to minimise this.Ĭentral Venous Catheter Placement Equipment Required Thrombus formation – this can cause complete occlusion of the catheter lumen(s) in severe cases, and careful management is required to prevent thrombosis.Ĭardiac arrhythmias may be seen at the time of catheter placement (usually self-limiting) Sepsis and/or cellulitis can result if they are improperly placed or managed. This is especially important at the time of placement, as this carries the highest risk of introducing contamination. These include:ĬVCs are not suitable for use in coagulopathic or thrombocytopenic patientsĬVCs are not suitable for patients with increased intracranial pressureĬVCs are not suitable for patients with wounds, cellulitis, vasculitis or other lesions in the region of the jugular veinĬVCs have a higher cost than standard cathetersĬVCs require more intensive monitoring and care, compared with peripheral catheters (24-hour care and monitoring must be available on-site)Ĭomplications associated with CVC use include:īacterial contamination – introduction of infection into the central circulation has more significant consequences than peripheral circulation. They are suitable for longer-term use than peripheral catheters – and can be left in situ for up to 14-21 days.ĬVCs do carry increased risks and special considerations when compared with standard peripheral IV catheters, and as nurses, we need to be aware of these to plan our nursing care effectively. 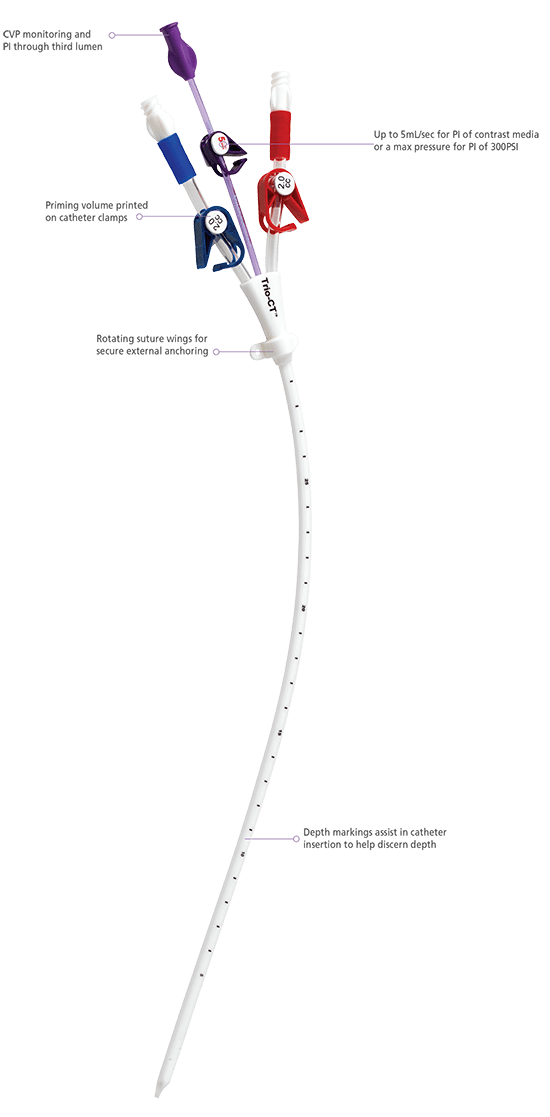
The administration of hyperosmolar solutions which would not be suitable for peripheral veins, due to an increased risk of phlebitis these solutions include concentrated glucose (>7.5%) solutions and parenteral nutrition solutionĪllowing measurement of central venous pressure (CVP)Ĭollection of multiple blood samples through the sampling port, without performing repeated venipuncture The administration of multiple (incompatible) agents at once through multi-lumen catheters (two or three separate lines, allowing for complete separation of incompatible substances through the same catheter) 
Why use one?ĬVCs have several benefits and specific indications, including: These are generally large-bore catheters and can be multi-lumen, allowing multiple fluids to be administered simultaneously. What is a central venous catheter?Ĭentral venous catheters (CVCs, or central lines) are catheters placed in such a way that the tip of the catheter sits in the vena cava. In today’s post, we’re talking all about what central venous catheters are, how they are placed, when to use (and when not to use!) them, and how to nurse the CVC patient. These are incredibly fun to place, allow us to administer multiple drugs and fluids easily, and collect samples without the need for repeated venipuncture - what’s not to like? One fantastic example of how we can do more to support our critical medical patients is through placing and maintaining central venous catheters. You folks know that if there’s one thing I’m passionate about, it’s us nurses doing more with our skills.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
